Links to other resources: Veterans Program, Medical Detox at Florida Springs
The 2025 “Pain in the Nation” report from Trust for America’s Health delivers a rare bit of hopeful news in the battle against substance abuse. Nationally, provisional data for 2024 suggest an unprecedented one-year decline of about 27 percent in drug overdose deaths. Alcohol-related deaths also dropped for the second year in a row. These are the largest decreases recorded in decades, signaling that some of the collective work being done in prevention, treatment, and harm reduction is beginning to bear fruit.
Yet, the report is clear that these improvements are not equally distributed. While some regions and communities are seeing rapid progress, others, particularly poorer and rural areas, have been left behind. Florida reflects this uneven reality, with certain parts of the state experiencing significant declines in mortality, while others continue to face entrenched problems. This is where local treatment centers like Florida Springs Wellness and Recovery Center in Panama City become crucial, as they serve communities that are often overlooked in the broader healthcare system.
National Progress and What’s Driving It
The downward trends in overdose and alcohol-related deaths are the result of several converging factors. Increased access to naloxone has saved lives in emergencies, while expanded use of medication-assisted treatment has helped people stabilize and begin recovery. Harm reduction programs, from fentanyl test strip distribution to syringe service initiatives, have become more widely available in many parts of the country. There has also been a greater integration of behavioral health into primary care and hospital settings, making it easier for patients to be identified and connected to support before a crisis escalates.
The Trust for America’s Health report also points to improvements in data tracking. Faster reporting systems mean health departments can detect spikes in overdose activity and respond quickly. These public health tools have allowed some states to deploy targeted interventions, such as surge outreach teams in areas experiencing sudden increases in drug poisonings.
However, the report warns that progress is fragile. Funding for public health programs is inconsistent, and workforce shortages in addiction treatment remain a critical barrier. Federal budget changes and shifting priorities could undermine the infrastructure that has supported these improvements.
Florida’s uneven recovery
Florida’s own overdose trends show a mixture of good news and continued concern. Statewide, preliminary numbers for 2024 appear to mirror the national decline, but the reductions are not uniform. Urban centers with robust public health funding and multiple treatment options have seen notable drops in mortality. By contrast, many rural counties, especially in the Panhandle and north-central regions, are still experiencing high rates of drug and alcohol deaths.
These rural areas face unique challenges. Healthcare provider shortages mean fewer local options for medical detox in Florida, and transportation barriers make it harder for residents to reach larger treatment facilities. Public health resources are spread thin, leaving little capacity for the kind of rapid response interventions that have helped drive down deaths in more populated parts of the state. Rural areas are also struggling with different drugs, as the graphic I show below entails. Panama City is in the types of areas that have seen increased overdoses from stimulants in recent years.
Poverty compounds the problem. Many individuals in these communities lack commercial insurance and depend on Medicaid or charitable care to access treatment. While Medicaid coverage for detox has expanded opportunities for care, not every facility accepts it, creating another obstacle for people in urgent need.
Florida Springs’ Role in Bridging the Gap
Located in Panama City, Florida Springs Wellness and Recovery Center is positioned at the heart of one of the state’s most underserved regions. The surrounding area includes a mix of small towns, agricultural communities, and coastal counties where substance abuse has taken a heavy toll. For residents here, options for drug and alcohol detox in Florida are limited, and Florida Springs serves as a vital link to recovery.
Florida Springs offers medical detox in Panama City that is fully equipped to manage withdrawal safely, followed by a continuum of care that includes inpatient and outpatient programs. This approach ensures that patients not only begin recovery in a medically supported environment but also have access to ongoing treatment tailored to their needs. For those using Medicaid coverage for detox, Florida Springs provides an affordable, accessible entry point into care without sacrificing quality.
Equally important, the facility is attuned to the realities of rural living. Outreach efforts extend into smaller communities, and transportation assistance can help patients overcome logistical barriers. By accepting a range of insurance plans and offering support for those with limited means, Florida Springs is reducing the equity gap that the national report identifies as a persistent challenge.
Why the Gains Haven’t Reached Everyone
The “Pain in the Nation” findings underscore that the improvements of the past two years are not universal. Several factors explain why rural and poorer areas lag behind in recovery outcomes:
- Limited access to medical detox and inpatient rehab
- Transportation barriers for those living far from major treatment hubs
- Lower availability of harm reduction programs such as naloxone distribution
- Economic instability that makes it harder for individuals to prioritize or sustain recovery
These disparities matter because they risk creating a two-tier system: one in which people in well-resourced areas can benefit from the latest interventions, while those in underserved regions continue to face high mortality rates.
The Path Forward for Florida’s Rural Communities
To ensure the progress of 2024 is not a short-lived success, the state will need to invest in strategies that bring treatment and prevention resources directly to underserved areas. This could include expanding telehealth capacity for addiction treatment in Florida, increasing mobile outreach teams, and providing additional funding for community-based recovery programs.
Facilities like Florida Springs can serve as regional anchors in this effort, working with local providers, law enforcement, and community organizations to coordinate care. By combining medical expertise with an understanding of the social and logistical barriers faced by rural residents, they can help ensure that the downward trend in drug and alcohol deaths reaches every corner of the state.
The national numbers from the “Pain in the Nation” report show that large-scale improvement is possible. The challenge now is to make sure those gains extend beyond the cities and into the smaller, poorer, and more remote communities that need them most.
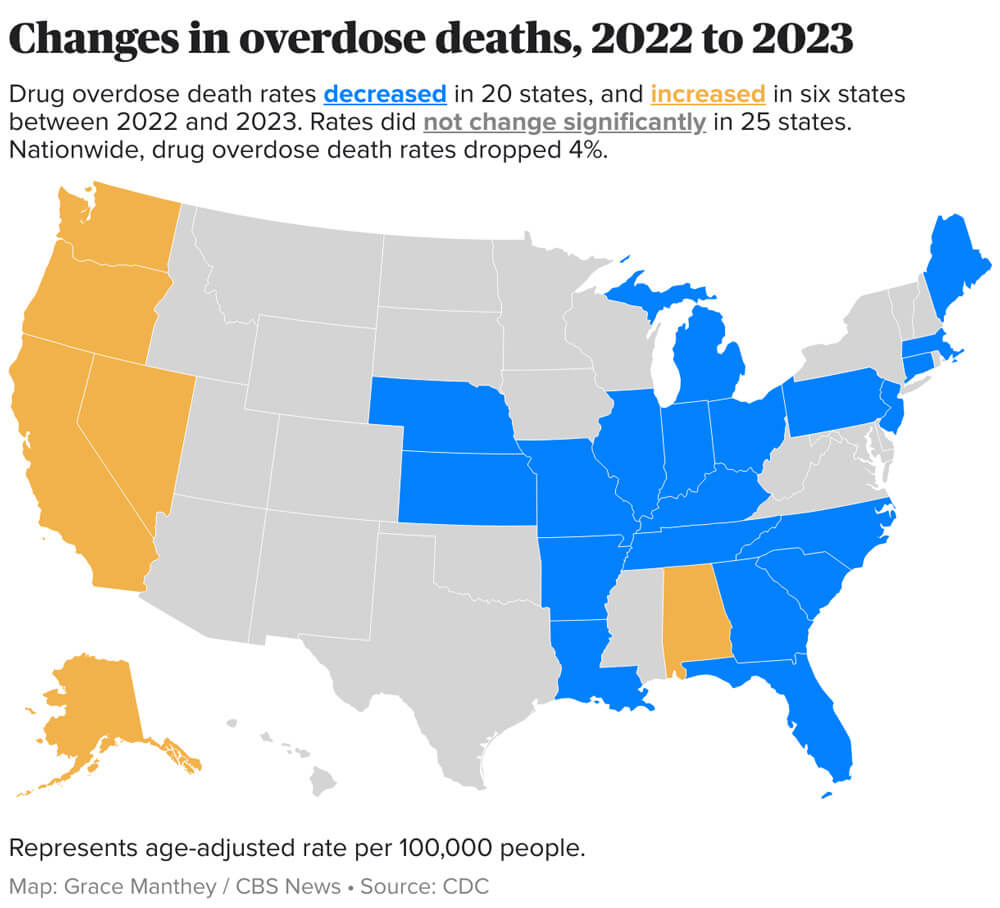
Here’s a national map highlighting the changes in overdose death rates from 2022 to 2023—including Florida’s nearly 10% reduction, shown in blue.
Overdose Map and Trend Insights for Florida (with Rural Context)
What the Map Shows
The visual above illustrates shifting overdose mortality rates across the U.S. between 2022 and 2023. Florida stands out with a significant decrease—from an age-adjusted rate of 35.2 per 100,000 in 2022 to 31.7 in 2023.
Florida-Specific Overdose Trends & Rural Disparities
State-Level Changes
- The reduction in overdose deaths in Florida mirrors the national trend of decline (4% nationally versus nearly 10% in Florida).
- As of early 2025, Florida’s overdose mortality remained higher than the national average, but the downward trajectory is hopeful.
Urban vs. Rural Disparities
- Nationwide, since 2020, urban counties had higher overall overdose death rates (28.6 per 100,000) compared to rural counties (26.2)
- However, specific drug categories reveal a more nuanced story:
- Synthetic opioids (e.g., fentanyl): Higher rates in urban areas.
- Psychostimulants (e.g., meth): 31% higher overdose rates in rural
By Tim Cannon